ALS is often called Lou Gehrig’s disease. In 1939, Lou Gehrig announced his retirement from the New York Yankees. He was only 36 years old as he told the crowd about his ALS diagnosis. He said, “For the past two weeks you have been reading about the bad break I got. Yet today I consider myself the luckiest man on the face of the earth.” Just two years later, he died.

ALS is a fast progressing motor neuron disease. This results in the wasting away of muscle, loss of movement and eventual paralysis. In general, ALS affects people between the ages of 40 and 70. 80% of people with ALS die within 2 to 5 years of diagnosis.
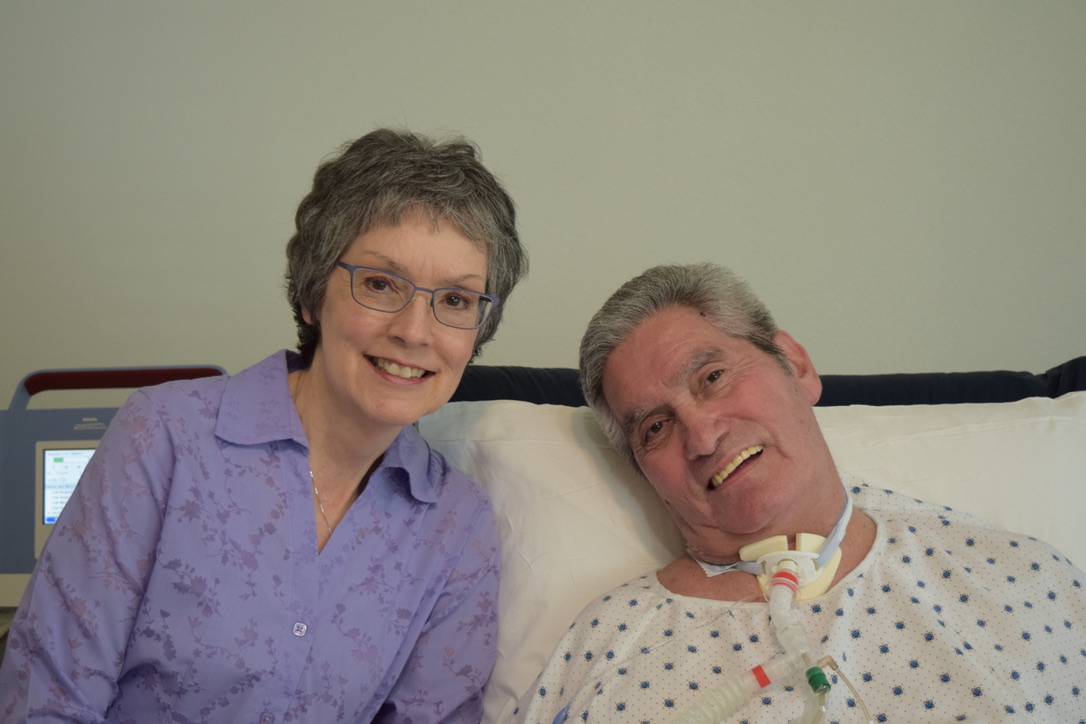
MY STORY “I feel invisible”, is one phrase my dad has mouthed to us time and time again over the past year. Three years ago, he could communicate with us through speaking and operate his laptop independently. Today, he cannot speak or move his arms/legs, and we communicate through lip reading.
Before ALS, my dad was a guitarist, singer and still is a lover of music. In 2016 at age 69, he was having trouble playing the guitar and then experienced drop foot and muscle twitches (fasciculations). He went through some testing, and the doctor initially said it was peripheral neuropathy. He had an EMG test done (tiny needles inserted into the muscles), and they found fasciculations consistent with ALS. The neurologist then proceeded to coldly tell my parents he had a death sentence, would eventually need a trach and would be placed on a breathing machine 24/7. This was extremely shocking for us, as it would be for anyone, and because of the harshness from this doctor, we all lived in denial for the following year. We didn’t believe his diagnosis and pursued other avenues. For a musician to lose all movement in his body was the worst possible scenario. It was devastating to imagine. Within a year, he needed oxygen, he had to use a walker, and the ALS diagnosis was feeling very real.
In 2018, my dad drifted off to sleep on the couch. We were unable to wake him and called an ambulance; we had no idea what was coming. The EMTs told us they needed to intubate him in the driveway because his airway had shut down and he was around 30% O2 saturation. Later we learned a slow decline in lung function is how ALS patients die from the disease. Because we called the ambulance and agreed to intubation, we were later faced with the decision to choose a permanent trach or allow him to pass. That was not a choice we wanted to make. It was devastating. The vent was keeping my dad alive, and we had to decide if he would live or die.
My dad chose the permanent trach, which places him on a vent for the rest of his life. At this point, we were confused, angry and in great disbelief. We assumed he would live in a facility far away because there are very few facilities in the country who accept patients on a vent and many are sub-par. After rehab in Austin and a short stay in a Temple, where he contracted an antibiotic-resistant pneumonia, the hospital said there was nothing they could do. My dad was going to die. Luckily, the VA took over and whisked him away to the VA Hospital in Temple. They were a God-send! After several months of being treated there, they trained us to care for him at home. We didn’t know we were capable of the things that were required for his care. But because of the VA’s persistence and God’s mercy, my dad has been home for 3 years now.
This is the hardest thing any of us have ever done. My mom spends her days and evenings doing his peg tube feeding, administering medication and caring for his needs. Both of them are weary. It is an emotionally heavy job, but we’re thankful to have him at home where we can spend time with him. My mom is a rockstar and my parents both get their strength from God. We couldn’t do this without God, our caregivers and the amazing help from the VA.


ALS has no cure, but there are treatments available! If you want to help, become an advocate to easily contact your representatives. Learn more about ALS so you can be prepared if this happens to your loved one.
EARLY SIGNS OF ALS
-muscle cramps, spasms or twitching in arms or legs
-weakness in hands and feet
-difficulty speaking or swallowing
I’m more than happy to answer any questions. The more knowledge we have, the more we can do to help others!